Although many people use the terms "headache" and "migraine" interchangeably, migraine is a distinctive disorder that causes a variety of symptoms. In addition to causing severe headaches, nausea, loss of vision and other symptoms, migraines also have a major impact on American workplaces. Olivia Begasse de Dhaem of Harvard Business Review reports that employees with migraines miss an average of 4.4 days of work each year. Migraines also cause employers billions of dollars in lost productivity and short-term disability claims.
Researchers haven't identified a specific cause of all migraine pain, but many people notice their symptoms worsen when they're more stressed out than usual. So, can stress cause migraines? It turns out that severe migraines from stress are extremely common. Read on to find out why stress triggers frequent migraine headaches and learn what you can do to reduce stress in your daily life.
What Causes Migraines?

Migraines have several common triggers, including stress, menstrual cycles, environmental changes and exposure to certain foods. According to researchers, approximately 70% of individuals with migraines report that stress triggers their symptoms. Potential environmental triggers include poor air quality, changes in barometric pressure, flickering lights, bright sunlight and exposure to strong odors. Onions, garlic, chocolate and foods containing nitrites or nitrates are some of the most common food-related migraine triggers.
Why Does Stress Trigger Migraines?

Researchers are still investigating the exact cause of migraines, but there's some evidence that this type of headache occurs as a response to changing brain chemicals. Serotonin, a chemical that helps nerve cells communicate with each other, plays a role in regulating pain. When serotonin levels decrease during times of anxiety, stress and depression, migraine headaches are more likely to occur.
Constant stress and anxiety also make it difficult for patients with migraines to get restful sleep and engage in other self-care activities, further increasing the release of stress hormones and risk of developing a migraine or recurrent headache. Surprisingly, relaxing isn't a surefire way to prevent chronic migraines. In some people, a period of relaxation after a period of intense stress creates a "letdown effect," triggering head pain and other migraine symptoms.
What Are the Symptoms of Stress-Induced Migraines?

Before a migraine headache begins, you may notice these general symptoms of stress:
- Fatigue
- Irritability
- Muscle aches
- Upset stomach
- Sadness
- Lack of interest in your usual activities
- Depression
- Elevated blood pressure
- Chest pain
Once a migraine starts, it typically develops in four phases: prodrome stage, aura development, headache phase and postdrome phase.
Prodrome Stage

The prodrome stage usually occurs about two days before you start experiencing migraine symptoms. During this phase, you may experience food cravings, constipation, neck stiffness, mood changes, frequent yawning and increased thirst.
Aura Development
Not everyone experiences auras, but if you do, you may notice aura symptoms before a migraine headache begins or once it's already in progress. For some people, auras are visual, resulting in vision loss or the appearance of bright spots in their field of vision. Other people report hearing unusual noises, one-sided weakness or numbness, difficulty speaking, uncontrollable movements or "pins-and-needles" sensations in the limbs. Each symptom varies person to person and typically lasts for up to one hour.
Headache Phase

The headache phase, also known as the migraine attack phase, is when you start to experience major migraine symptoms. Such an attack typically lasts anywhere from four to 72 hours. During this time, you may experience any of these symptoms:
- Pain on one or both sides of the head
- Nausea and vomiting
- Sensitivity to light and noises
- Throbbing or pulsating pain
- Sensitivity to touch or smell
Postdrome Phase
Think of the postdrome phase as a migraine "hangover." You may feel confused or fatigued for up to a day after the headache phase ends. Some migraine patients also experience intermittent pain when making sudden head movements.
7 Ways to Find Relief From Stress-Induced Migraines
1. Stress Management
This may seem obvious, but the best way to prevent stress-induced migraine headaches is to reduce stress in your daily life. Take care of your mental wellness by improving your sleep hygiene, studying relaxation therapies, eating well and getting plenty of regular exercise. Sleep hygiene refers to the steps you take to get high-quality, uninterrupted sleep each night. The Sleep Foundation recommends waking up at the same time each day, dimming your lights in the evening and discontinuing electronic use at least 30 minutes before you go to bed. Yoga and meditation can also help you eliminate stress and reduce your risk of stress headaches.
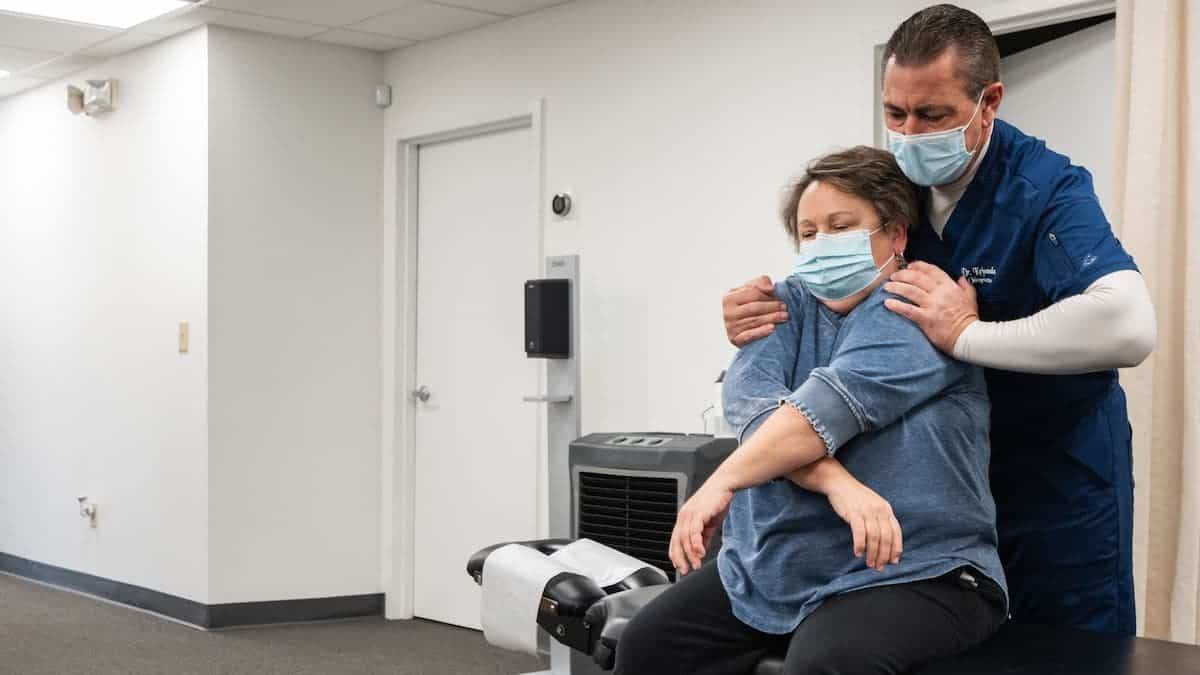
2. Chiropractic Care

If migraine stress management isn't reducing the number of migraines you experience each month, visit an experienced chiropractor. Realignment of the spine stimulates the nervous system and makes it easier for your brain to communicate with other parts of your body, reducing the risk of chronic migraines. Chiropractic care also reduces stress by improving circulation and easing muscle tension.
According to researchers from Harvard Medical School and Brigham and Women's Hospital, chiropractic treatment may improve therapeutic outcomes in people with migraine headaches. Study investigators discovered that traditional migraine treatment paired with chiropractic spinal manipulation resulted in improved pain scores and reduced reliance on pain-relieving medications.
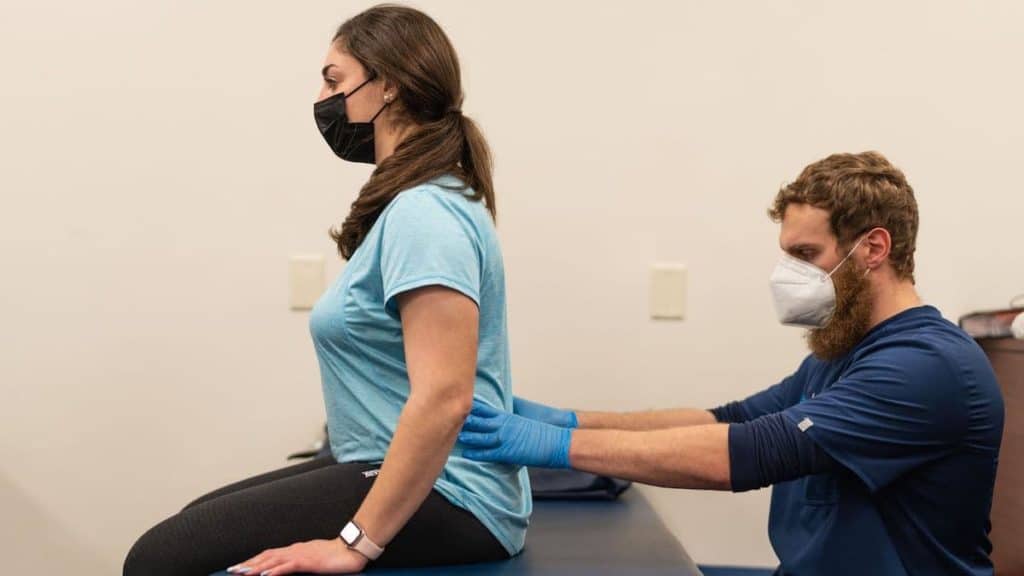
3. Physical Therapy
Tense muscles can result in vasodilation, or dilation of the blood vessels. Vasodilation has been linked to an increased risk of migraines, making it important to address muscle tension as soon as it develops. Physical therapy eases muscle tension and has several other benefits for people with a history of migraines. For example, physical exertion performed throughout PT stimulates the autonomic nervous system, which controls blood pressure, heart rate, respiration and other important processes. Treatment plans help ease stress and anxiety, reducing the likelihood of having a migraine. During a physical therapy session, you may even learn some breathing techniques to reduce your stress level even further.
4. Acupuncture Therapy

During an acupuncture session, a trained practitioner inserts thin needles at specific points on your body. Needle insertion stimulates the nervous system, triggering the release of natural painkillers called endorphins. These are the same "feel-good" chemicals released by your brain when you exercise.
Acupuncture is also helpful for reducing chronic stress, as it gives you a chance to lie down in a calm environment, listen to music and relax while the practitioner administers your treatment. The needles are so thin that they cause no pain, allowing you to reduce your risk of common migraines without undergoing invasive medical treatments. Best of all, acupuncture is effective. Dr. Albrecht Molsberger of the Center for Sensory Disorders reports that acupuncture treatment works just as well as prophylactic medications as a preventive treatment for migraines.
5. Massage Therapy
Massage therapy doesn't just feel good; it can also help reduce the number of migraines you experience in any given month. During a massage, the therapist's hand movements increase blood flow to the muscles, reducing muscle tension. Massage is also incredibly relaxing, helping to reduce chronic stress, as each session typically takes place in a dim, quiet room with white noise or calming music playing in the background. Massage therapy also reduces the amount of cortisol circulating in your blood. Cortisol, known as the "stress hormone," increases your blood pressure and heart rate, contributing to the high levels of stress that can trigger migraines.
6. Behavioral Therapy

If you're going through a rough patch and have more stress than you can handle on your own, consider meeting with a behavioral therapist. Behavioral therapy gives you a chance to discuss the stressful circumstances in your life with an unbiased person who can make practical recommendations for improvement. Your therapist may also be able to help you improve your coping skills and change negative thought patterns into positive ones, making it easier to manage stress when it arises.
It's not possible to eliminate every source of stress from your life, but behavioral treatments can help you change the way you react to stressful situations. As a result, seeing a therapist may help you prevent migraines or reduce their frequency.
7. Medications
Many people prefer to use drug-free treatment options, but you may want to try medications to prevent migraine attacks or manage your symptoms once a migraine begins. Prophylactic medications, also called preventive medications, are typically recommended for people who have at least two migraines per month. These preventive medications aim to improve your quality of life by reducing the frequency and severity of your attacks. Propranolol, divalproex, amitriptyline and topiramate are some of the first-line therapies used to prevent migraines.
If you can't stop an attack before it starts, there are over-the-counter medications available to relieve your symptoms. Ibuprofen, naproxen sodium, acetaminophen and aspirin combined with caffeine are some of the most common OTC options. Be sure to take migraine medications according to the instructions and consult your healthcare provider about ongoing usage.
Stop Migraines at the Source With Northeast Spine and Sports Medicine
Northeast Spine and Sports Medicine is a multidisciplinary practice, meaning you can access multiple medical specialties in one convenient location. In addition to our experienced physicians, we have skilled chiropractors, physical therapists and acupuncturists available to address your symptoms and help you get relief from stress-induced migraines.
To learn more about our expertise and the services we provide, contact Northeast Spine and Sports at (732) 653-1000 or book an appointment online. We look forward to helping you get relief from headaches, nausea, visual disturbances and other migraine symptoms.