Nearly 80% of people experience back pain at some point in their lives. Some individuals may experience only fleeting pain but for others, the condition can result in lost wages, costly medical bills and a reduced ability to participate in regular activities. However, safe, effective treatments — such as spinal decompression therapy — can relieve or reduce back pain, helping many sufferers return to a pain-free life.
What Is a Spinal Decompression Procedure?
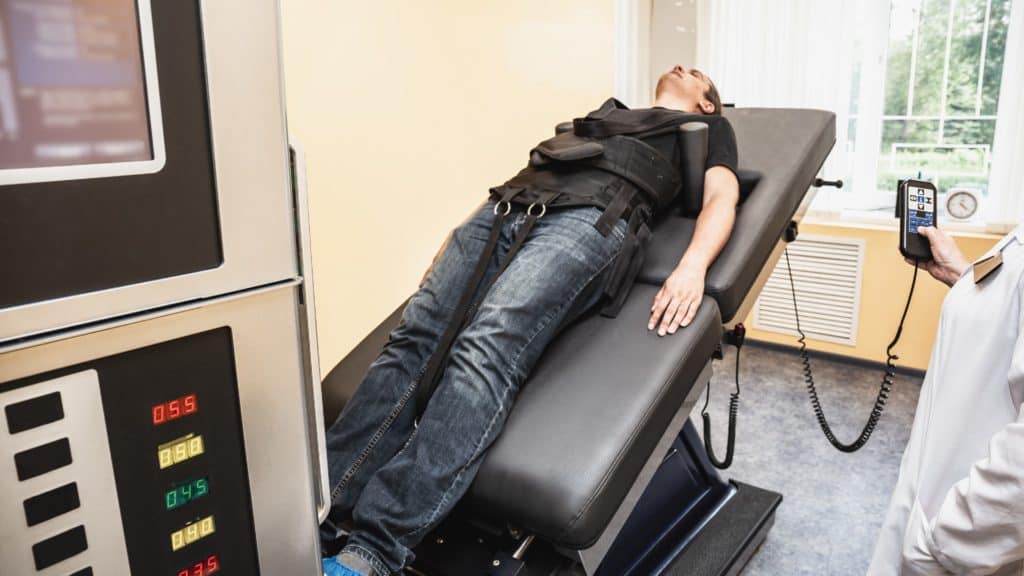
Chiropractors and other trained pain management professionals use non-surgical spinal decompression therapy to relieve back pain caused by pressure on the spinal cord or a compressed nerve root. Developed in the late 1900s by Dr. Allan Dyer, this noninvasive technique is similar to traction therapy. It uses a specialized traction table or motorized device to gently stretch a patient's spine, taking pressure off their spinal disks. The reduced pressure can cause herniated or bulging disks to retract, further relieving the pressure on spinal structures and associated nerves to promote healing and reduce back, neck and leg pain.
Who Benefits From Spinal Decompression?

Because it's fast-acting and minimally invasive, spinal decompression is often one of the first therapies prescribed for individuals suffering from spine-related back, leg or neck pain. The procedure may benefit patients who’ve been diagnosed with:
- Sciatica
- Spinal stenosis
- Pinched nerves
- Degenerative disk disease
- Bulging or herniated disks
- Posterior facet syndrome
- Diseased or damaged spinal nerve roots
How Does a Doctor Decide Whether Spinal Decompression Is Recommended?
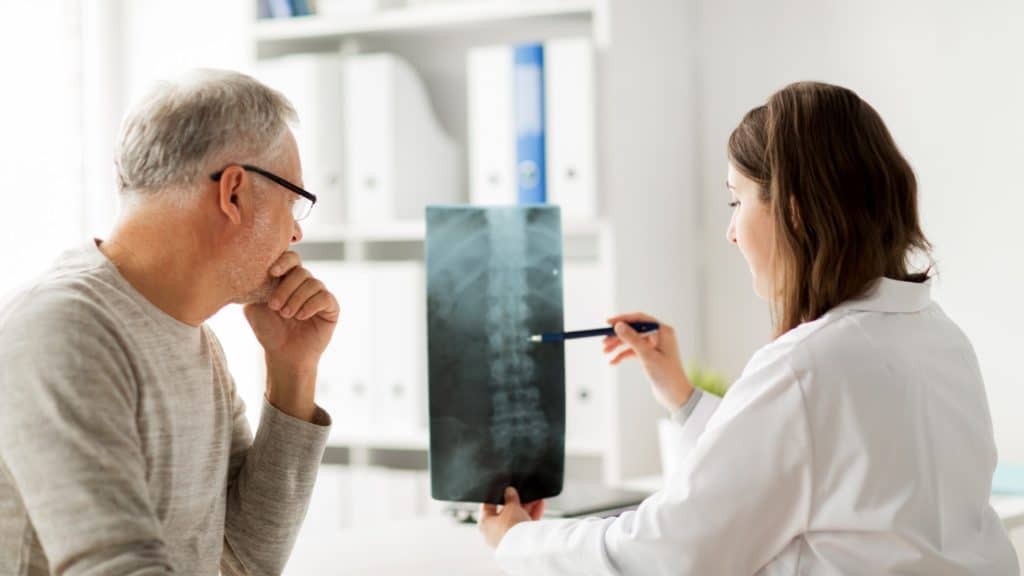
To assess whether spinal decompression is the best course of treatment for a patient, a healthcare practitioner needs to better understand the disease or injury. To do so, they'll typically evaluate the level and duration of a patient's pain, test the functionality of specific joints and muscles and ask about any other relevant symptoms. For a complete picture of a patient's medical needs, a healthcare provider may also perform one or more diagnostic tests, including:
- Bone scans
- X-rays
- MRIs
- CT scans
- Nerve conduction studies
Once the results of all relevant diagnostic tests are in, the practitioner may assess whether spinal decompression therapy is clinically appropriate and schedule treatment if it is.
What Happens During a Spinal Decompression Procedure?

During a spinal decompression procedure, a trained healthcare professional fits supports around the patient’s trunk and pelvis. These harnesses secure the patient to the treatment table to ensure their safety. Depending on an individual's diagnosed condition, they may be asked to lie face down or face up on a motorized table. Patients remain fully clothed during the procedure.
Once the patient is positioned appropriately, the practitioner begins to separate the two parts of the table to gently stretch the individual's spine. Typically, the upper half of the table remains in place while the lower half slides out to stretch the spine. This manipulation may be done manually or by using a computer.
Stretching may be alternated with periods of relaxation, and the treatment can be tailored to meet an individual’s specific medical needs. Patients are constantly monitored, and the practitioner may adjust the treatment as needed to prevent muscle spasms. Motorized tables often come with a patient safety switch, which lets them stop the procedure immediately if they experience discomfort or anxiety.
Spinal decompression therapy is often used alongside other types of pain mitigation treatments, including:
- Ultrasound
- Acupuncture
- Physical therapy
- Electrical stimulation
- mild® procedure
- Heat or cold therapy
- Prescription muscle relaxants
- OTC or prescription pain relievers
What Does Spinal Decompression Do to Your Body?

Spinal decompression therapy gently stretches the spine, altering its position and taking pressure off the spinal disks that cushion the vertebrae. This creates negative pressure within the disk, causing herniated or bulging disks to retract and lessening the stress on spinal structures and associated nerves. As a result, patients may experience increased blood flow, and oxygen, water and nutrient-rich fluids can move more easily into the disks to promote healing.
What Can You Expect After a Spinal Decompression Procedure?
Some patients experience pain relief after just one spinal decompression treatment. However, patients may require as many as 20 sessions over a 4- to 6-week period to achieve long-lasting pain relief.
Patients who undergo non-surgical spinal decompression treatments don't typically experience serious side effects. However, some individuals may experience muscle soreness or backaches following the procedure. These sensations are usually mild and short-lived and occur less frequently as treatment progresses.
Frequently Asked Questions

What does spinal decompression feel like?
During a spinal decompression treatment, patients may feel their spine gently stretching and relaxing. Many patients find the therapy relaxing and fall asleep during the session. However, individuals who have severely damaged disks may have mild discomfort during the first few treatments.
How long does a spinal decompression session last?
A spinal decompression session typically lasts between 30 and 45 minutes. However, patients often require multiple sessions to achieve optimal results.
Can spinal decompression hurt you?
Spinal decompression is a painless, noninvasive procedure that has a low risk of side effects. However, this therapy isn’t recommended for individuals who are pregnant, take blood thinners or have been diagnosed with any of the following conditions:
- Tumors
- Spinal fractures
- Broken vertebrae
- Advanced osteoporosis
- Abdominal aortic aneurysms
Individuals who’ve undergone spinal fusion surgery or who have metal implants in the spine should also forego spinal decompression therapy.
Is spinal decompression used to treat other conditions?
Spinal decompression is most commonly used to treat spine-related back, neck and leg pain and headaches. However, some individuals may pursue treatment as part of a comprehensive wellness strategy or to improve energy and enhance the body’s immune response.
Are there other types of spinal decompression treatments?
Yes. Spinal decompression is often used as an umbrella term for therapies and treatments, including surgical procedures, that provide relief from back pain by reducing pressure on an individual’s spine. Surgical options typically involve the removal of bone or other tissue to open the spinal canal and relieve pressure on nerves. They may include:
- Osteophyte (bone spur) removal
- Removal of a vertebra
- Partial or full disk removal
- Expansion of the openings housing the nerve roots
- Removal of some or all of the bony arches on the spinal canal
Some of these procedures may be performed in conjunction with spinal fusion surgery to increase a patient's spinal stability and further reduce pain.Spinal decompression therapy can be a safe, fast-acting treatment for individuals suffering from compression-related neck, back and leg pain. NorthEast Spine and Sports Medicine’s experienced pain management team can assess your back pain and help you choose a treatment plan that'll put you on the path to a pain-free life. Book an appointment for a consultation today.